A well-crafted medical director job description is your first move in attracting a leader who can walk the tightrope between clinical excellence and strategic oversight. This senior physician acts as the bridge connecting hands-on patient care with high-level business strategy, making sure the entire organization hits its quality and safety targets.
What Does a Medical Director Actually Do?

Think of the Medical Director as the chief architect of a healthcare organization's clinical quality. While frontline physicians zero in on individual patients, the Medical Director designs and oversees the entire system that ensures every patient gets the best possible care. They are the ultimate guardians of clinical integrity, blending deep medical expertise with executive leadership.
This job isn't just about managing other doctors; it's about steering the organization's entire clinical ship. They're the ones developing medical policies, ensuring protocols are evidence-based, and nurturing a culture of continuous improvement across the medical staff. Their work is also absolutely critical for staying compliant with regulatory bodies like HIPAA and CMS.
The Four Pillars of the Role
When you break it down, the Medical Director's function rests on four fundamental pillars. Getting these right is the key to writing a job description that attracts candidates with the perfect mix of skills.
The role of a Medical Director is a unique synthesis of clinician, administrator, strategist, and mentor. They must be as comfortable discussing complex patient cases as they are analyzing departmental budgets and performance metrics.
This unique combination of duties makes the position both incredibly challenging and highly valued. The compensation certainly reflects that, with the average salary for a Global Medical Director hovering around $232,369 per year. Of course, that figure can swing pretty wildly based on location, experience, and the organization's size, with top earners pulling in over $334,500 annually.
To give you a clearer picture, this table breaks down the core functional areas that truly define this critical position. It’s a great starting point for both hiring managers and aspiring leaders.
Core Pillars of the Medical Director Role
| Pillar | Core Function | Example Activities |
|---|---|---|
| Clinical Governance | Upholding the standard of care | Developing clinical protocols, leading quality assurance initiatives, and overseeing patient safety programs. |
| Staff Leadership | Guiding and mentoring clinicians | Conducting performance reviews, managing physician credentialing, and resolving interpersonal conflicts. |
| Regulatory Compliance | Ensuring adherence to all laws | Monitoring changes in healthcare law, preparing for audits, and implementing HIPAA-compliant practices. |
| Strategic Planning | Aligning clinical and business goals | Participating in budget creation, advising on new service lines, and championing new medical technologies. |
These pillars show just how multifaceted the role is, demanding a leader who can operate on multiple fronts simultaneously.
For anyone looking to step into a position like this, understanding these different facets of medical leadership is the first crucial step. If that's you, you might find our collection of articles on the medical director career path helpful.
Breaking Down Key Responsibilities and Duties

Being a medical director is about much more than a title on an office door. It’s a dynamic role that sits at the intersection of high-level strategy and ground-level execution, demanding a sharp blend of clinical expertise and operational leadership.
The responsibilities listed in a job description aren't just a checklist; they form a blueprint for how the organization safeguards patient care and drives its clinical vision forward. These duties generally fall into a few key areas, and understanding them is crucial to grasping the true scope of the job.
Clinical Governance and Quality Assurance
At its heart, the medical director is the ultimate guardian of clinical quality. This means setting the standards of care that every single provider in the organization must meet. Think of them as the conductor of a clinical orchestra, ensuring every professional plays their part in harmony to deliver the best possible patient outcomes.
This domain covers things like:
- Developing and Enforcing Protocols: They are responsible for creating evidence-based clinical guidelines and, just as importantly, making sure they’re applied consistently across the board.
- Overseeing Quality Improvement: This involves leading initiatives to reduce medical errors, improve patient safety, and elevate the overall patient experience. For example, a director might champion a new sepsis detection protocol after analyzing patient data and identifying a gap.
- Managing Peer Review: They establish a fair, constructive process for reviewing physician performance and addressing any concerns about clinical practice before they become larger problems.
Staff Leadership and Mentorship
A great medical director doesn’t just manage—they lead and inspire. They are directly responsible for the professional growth and performance of the medical staff, serving as a mentor, coach, and, when necessary, a firm hand. It requires a delicate balance of strong leadership and deep empathy.
A medical director must cultivate a culture where clinical excellence can thrive. They set the tone for collaboration, continuous learning, and unwavering accountability among the medical team.
For instance, when a complex new medical technology is introduced, the director leads the charge. They oversee the training, adoption, and integration, making sure the team feels supported rather than overwhelmed by the change. This part of the job also includes handling physician credentialing, performance evaluations, and conflict resolution to foster a positive, productive work environment.
Regulatory Compliance and Risk Management
Navigating the labyrinth of healthcare regulations is a massive part of the job. The medical director ensures the organization follows every rule set by bodies like HIPAA, CMS, and The Joint Commission. They essentially act as the organization's compliance compass, always pointing toward ethical and legal best practices.
This involves staying on top of constantly changing healthcare laws and preparing the organization for surprise audits and inspections. If a potential compliance issue arises—like a patient data privacy concern—the director spearheads the investigation and implements corrective actions to mitigate risk.
The financial weight of this oversight is significant. Data shows that medical directors earn an average salary of about $204,000 annually, a figure that reflects the high stakes of their work. You can find more insights on medical director salary trends and job requirements to see how this varies by location and specialty.
Essential Qualifications and Skills for a Medical Director

When you're writing a job description for a medical director, you're not just looking for a qualified candidate. You're looking for a transformative leader.
This role demands a rare combination of deep clinical expertise and savvy business sense. The right person has to be just as comfortable in the exam room as they are in the boardroom.
The path to becoming a medical director is a long one, built on years of demanding medical training and hands-on clinical work. That experience isn't just a checkbox; it's the bedrock of the credibility needed to lead a team of highly skilled physicians.
The Educational and Experiential Foundation
Before you even get to the leadership skills, there are some non-negotiable qualifications. Think of these as the absolute table stakes for anyone who wants to be considered.
- Medical Degree (MD or DO): The journey starts here, with a degree from an accredited medical school.
- Active State Medical License: A candidate must hold a current, unrestricted license to practice medicine in the state where they'll be working.
- Board Certification: This is key. Certification in a specific medical specialty demonstrates a proven, high level of expertise in their field.
- Extensive Clinical Experience: Most organizations are looking for a minimum of 5+ years of clinical practice after residency. Often, they’ll want to see 3+ years in some kind of leadership or administrative role, too.
This progression ensures a medical director has actually walked the walk. They understand the daily grind and the real-world challenges their medical staff face every day.
A medical director's authority comes from more than just a title. It's earned through years of clinical excellence and a demonstrated commitment to patient care. They have to be a clinician first, manager second.
Bridging Clinical Practice with Business Leadership
Once you get past the diplomas and licenses, the best medical directors have a sophisticated mix of hard and soft skills. This is what allows them to translate clinical needs into operational strategy and steer their teams toward the organization's goals.
The hard skills are the more technical, administrative abilities. This means having a solid grasp of financial management to handle budgets, knowing your way around data analysis to track clinical outcomes, and understanding electronic health record (EHR) systems inside and out.
But it’s the soft skills that really separate a good leader from a great one. These are the interpersonal abilities that drive influence and create real change.
- Communication: Can they articulate a clear vision to clinicians and executives alike?
- Conflict Resolution: Are they skilled at mediating disputes between staff or departments?
- Emotional Intelligence: Do they understand team dynamics and lead with empathy?
- Strategic Thinking: Can they connect clinical initiatives to the bigger business objectives?
This combination is absolutely critical. In fact, understanding why every healthcare leader needs business skills is a game-changer for any aspiring director. The ability to speak the language of finance and operations is what empowers a clinical leader to fight for resources, get buy-in, and drive meaningful improvements for their teams and patients.
How Setting and Specialty Shape the Role
The title “Medical Director” isn't a one-size-fits-all role. Far from it. A medical director leading a hospice facility has a fundamentally different job than one steering clinical trials at a pharmaceutical company.
The specific environment—whether it's a bustling hospital, a data-driven insurance firm, or a fast-moving biotech startup—radically changes the focus, responsibilities, and strategic priorities of the position.
Think of it like being a chef. A chef in a high-end French restaurant obsesses over intricate techniques and classic flavors. A chef running a food truck, on the other hand, prioritizes speed, efficiency, and bold, simple dishes. Both are masters of their craft, but their daily tasks and what defines success are worlds apart. It’s the exact same story for a medical director.
Contrasting Priorities Across Healthcare Sectors
In a hospital, the medical director is deep in the trenches of day-to-day clinical operations. Their world revolves around patient safety protocols, physician performance management, and making sure the institution is compliant with bodies like The Joint Commission. They're focused on improving care quality within the four walls of their facility.
Now, shift gears to a medical director at an insurance company. They operate at a much higher altitude. Their focus zooms out to population health, utilization management, and developing medical policies that guide coverage for thousands, even millions, of members. They spend their time analyzing large-scale data to spot trends, not overseeing individual patient cases.
The core duties in a medical director job description might look similar on paper, but the real-world application is dictated entirely by the organization's mission. One role centers on compassionate end-of-life care protocols, while another is consumed by the rigorous demands of regulatory submissions for a new drug.
This table breaks down how the role shifts across different healthcare settings.
Medical Director Role Variation by Organization
| Setting | Primary Focus | Key Skills Emphasis |
|---|---|---|
| Hospital System | Patient safety, clinical quality improvement, physician management, and regulatory compliance (e.g., Joint Commission). | Clinical leadership, operational efficiency, interpersonal communication, and quality assurance. |
| Insurance Company/Payer | Population health management, utilization review, medical policy development, and network adequacy. | Data analysis, policy writing, risk management, and understanding of reimbursement models. |
| Pharmaceutical/Biotech | Clinical trial oversight, drug safety (pharmacovigilance), regulatory submissions (FDA), and medical affairs strategy. | Scientific research, regulatory affairs, project management, and strategic marketing support. |
| Hospice/Palliative Care | End-of-life care protocols, symptom management, family support, and interdisciplinary team leadership. | Compassionate communication, ethical decision-making, team collaboration, and care planning. |
| Ambulatory Surgery Center | Surgical quality outcomes, credentialing of surgeons, infection control, and operational efficiency. | Clinical governance, process optimization, risk assessment, and peer review. |
As you can see, while the "Medical Director" title is constant, the job itself is a chameleon, adapting to its environment.
The Impact on Compensation and Career Path
This massive variation in responsibility also directly influences compensation and career progression. The skills needed to thrive in a biotech firm are different from those required in a stable hospital system, and salaries reflect that demand. Experience, of course, plays a huge role in this equation, with pay scaling significantly as a director's career advances.
The data below shows just how much compensation, including salary and bonuses, can evolve with experience.
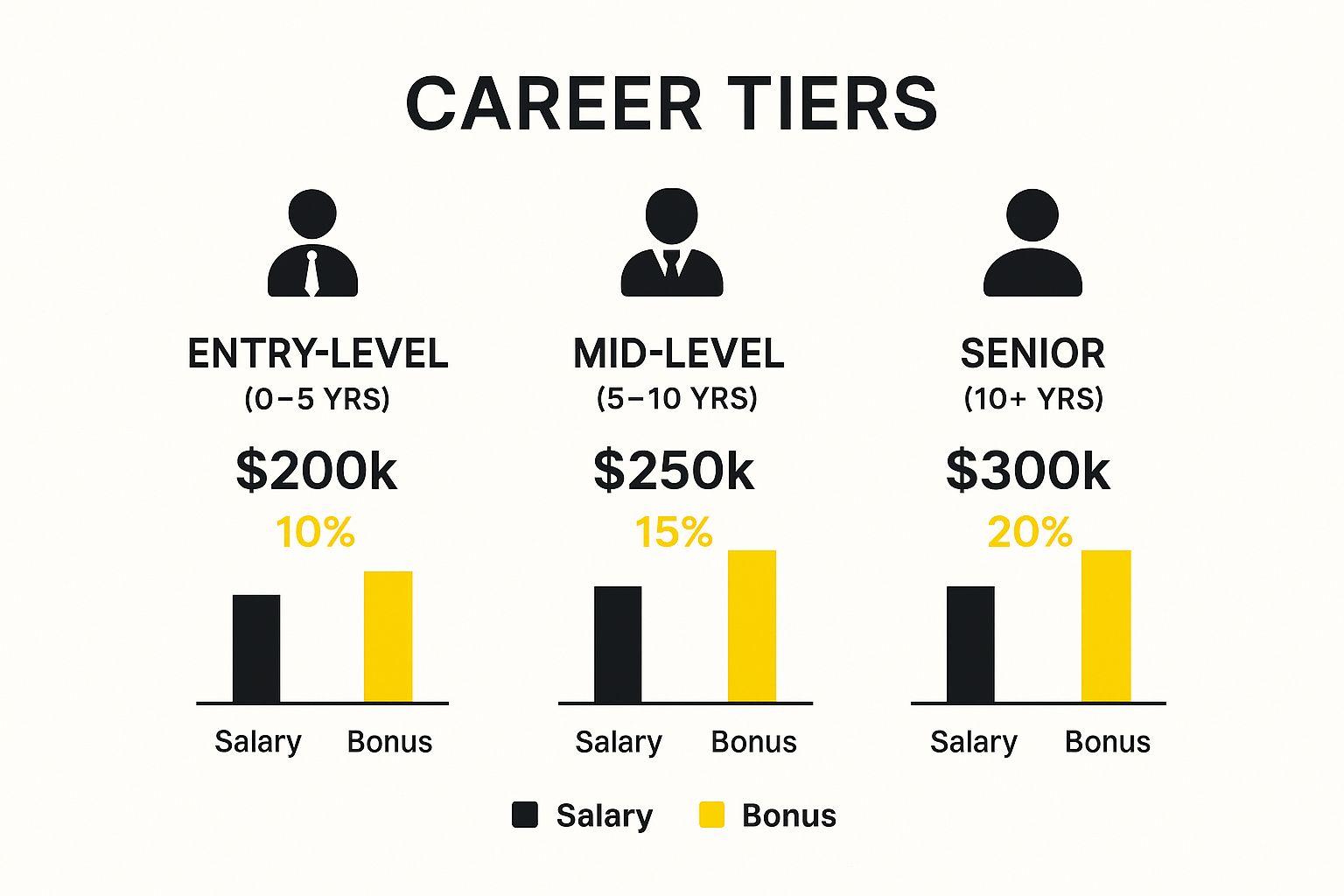
There’s a clear, strong correlation between years in the field and earning potential. Senior roles command substantially higher financial rewards because the scope of responsibility expands from pure clinical oversight to high-stakes strategic leadership.
This progression is backed up by broader industry data. The average salary for medical directors in the U.S. lands around $230,206, but that number is heavily skewed by experience. For example, early-career directors with 1–4 years under their belt earn an average of $178,302. At the senior level, it’s not uncommon to see salaries soar well over $300,000. If you want to dig into the numbers, you can explore more about how experience and specialty affect medical director pay and see a more detailed breakdown.
How to Write a Medical Director Job Description
Crafting a job description for a medical director is less about listing tasks and more about telling a compelling story. This isn't just an HR document; it's your primary tool for attracting elite clinical leaders. It needs to be precise, engaging, and a genuine reflection of your organization's mission and culture.
Think of it as a blueprint for your ideal candidate. A good one not only details the role's architecture but inspires the right person to want to build with you. A generic, copy-pasted description will only attract generic candidates. The best ones are looking for a role that resonates with their professional values and truly challenges their skills. Your goal is to create a document that acts as both a filter and a magnet—screening for the right qualifications while pulling in top-tier talent who see themselves in your vision.
Start with a Powerful Job Summary
The first paragraph is your hook. It has to grab the essence of the role and the opportunity in just a few sentences. Forget the dry overview. Instead, paint a picture of the impact this medical director will have on your organization and the community you serve.
- Go Beyond the Basics: Don't just say, "We're hiring a medical director." Try something more engaging, like, "We are seeking a visionary clinical leader to spearhead our commitment to exceptional patient care and guide our medical staff through an exciting phase of growth."
- Highlight Your Mission: Briefly connect the role to what you do best. Are you focused on innovative cancer research? Community health equity? Pioneering new surgical techniques? Mention it.
A job description is a marketing document. Your first objective is to sell the opportunity. The best candidates have options; you need to show them why your role is the one they should choose.
This initial summary sets the tone. It gives a busy physician leader a compelling reason to keep reading.
Detail Responsibilities with Action-Oriented Language
When you get to the core duties, use strong, active verbs. This makes the role feel dynamic and clearly communicates what you expect. Ditch passive phrases like "responsible for" and lead with words like "drive," "develop," "oversee," "mentor," and "champion."
Organize the responsibilities into logical buckets to make the information digestible. These categories should mirror the key pillars of the role itself.
- Clinical Governance and Strategy: This is where you describe the high-level duties. For example: "Drive the development and implementation of evidence-based clinical protocols to enhance patient safety and outcomes."
- Medical Staff Leadership and Development: Focus on the people part of the job. For instance: "Mentor and guide a team of dedicated physicians, fostering a culture of collaboration, continuous learning, and clinical excellence."
- Regulatory Compliance and Quality Assurance: Make their role as a guardian of standards crystal clear. Example: "Oversee all quality assurance programs and ensure unwavering compliance with HIPAA, CMS, and Joint Commission regulations."
This structure helps candidates quickly size up the scope and focus of the position.
Clearly Define Qualifications and Reporting Structure
Be absolutely explicit about the must-haves versus the nice-to-haves. This section should clearly list the non-negotiables—like an MD or DO degree, board certification, and a specific number of years in both clinical practice and a leadership capacity.
It's just as important to define the reporting structure. State clearly who the medical director reports to, whether it's the Chief Medical Officer (CMO), CEO, or another executive. This kind of transparency helps candidates understand where they fit within the organizational hierarchy and sets clear expectations from day one. A well-defined structure shows you have a clear plan for how this critical leader will integrate into your team.
Common Questions About Medical Director Roles
So, what does the path to a medical director role actually look like? What’s the day-to-day grind, and what are the real challenges that keep these leaders up at night? Let's break down some of the most common questions from aspiring leaders and the organizations trying to hire them.
The journey doesn't start with a director title. It begins years earlier, right after residency, with solid clinical practice. Most physicians don’t just jump into a formal leadership role; they ease into it. They might chair a hospital committee or step up as a department lead, quietly building the administrative muscle they'll need later. You can learn more about the specific steps and insider moves needed to make this transition in our dedicated guide on how to become a medical director.
Balancing Clinical and Administrative Duties
One of the biggest questions is always about the time split. How much of the job is seeing patients versus sitting in meetings? Honestly, it varies wildly.
In a large hospital system, a medical director might be 80% administrative and only 20% clinical, focusing almost entirely on strategy, oversight, and big-picture initiatives. But in a smaller practice, that director could easily be running a 50/50 split, staying deeply connected to hands-on patient care.
The modern medical director must be a master of the context switch—moving seamlessly from a patient consultation one moment to a high-stakes budget meeting the next. This agility is the true hallmark of an effective clinical leader.
The role today is also packed with pressure. Directors are wrestling with a tough, complex environment defined by:
- Navigating the constant churn of healthcare regulations.
- Tackling widespread physician burnout and critical staff shortages head-on.
- Integrating new tools like AI and telehealth without disrupting workflows.
- Balancing razor-thin budgets against unrelenting demands for high-quality care.
These challenges demand a leader with serious resilience and a sharp, strategic mind.
Not ready for a full-time medical director search? Fractional Medical Director roles — part-time, interim, or project-based — are a growing entry point for physicians building their executive career. Learn more at ClinX Academy: Fractional Medical Director.
Are you a clinician ready to step into a leadership role but lack the business background? The ClinX Academy Mini Healthcare MBA provides the practical business fluency you need to confidently transition into roles like medical director. Learn more at https://www.clinxacademy.com.